It is estimated that 20 million Americans have a thyroid problem, and that 12 percent of the general population will develop a thyroid disease in their lifetime. (1)
Those numbers only continue to grow. Autoimmune hypothyroidism, or Hashimoto’s thyroiditis, is the most common autoimmune disorder that exists, primarily affecting women.
So what is causing the little butterfly organ at the base of the neck to be such a widespread problem?
Are you struggling with a Thyroid condition? We’ve created a FREE guide that shows you how you can heal your thyroid.
Click here to get your FREE copy of our Thyroid Guide!
The Thyroid: What It Is and What It Does
The thyroid is a small endocrine, or “hormone producing,” gland that sits at the base of the throat, with two “wings” that sit on either side of the windpipe.
The thyroid is responsible for producing triiodothyronine (T3) and thyroxine (T4), the two main thyroid hormones. T4 is the inactive reserve form that is converted to T3 as the body needs it for energy and metabolism. The thyroid makes hormones when prompted from the pituitary gland, which is located in the brain.
The thyroid is well known for being associated with metabolism, but it is responsible for much more than just the ability to lose weight. While it does regulate how the body uses energy – which is why a low-functioning thyroid can have symptoms of extreme fatigue, and those with an overactive thyroid might experience restlessness or an inability to sleep – the thyroid also influences how effectively the brain, heart, muscles, liver, adrenal glands, and reproductive organs function.
How the Thyroid Gets Messed Up

It is possible for people of any age or gender to experience thyroid problems, but the most common issues are seen in women over the age of 30.
Typical triggers for thyroid disease include:
- Infection with a virus such as Epstein-Barr, cytomegalovirus, or certain members of the herpes virus family
- Genetics, including a family history of anyone with an autoimmune disorder of any kind or thyroid problems
- Pregnancy and postpartum changes
- Environmental triggers like toxins or chemical exposure
- Food allergy or sensitivity
- Effects from another autoimmune or chronic condition, like celiac disease, rheumatoid arthritis, multiple sclerosis, or fibromyalgia
While there may be other causes of an initial onset of thyroid disease, these are the most commonly found.
Hyperthyroidism and Graves’ Disease
Hyperthyroidism occurs when the thyroid produces too many hormones, resulting in cells that are overstimulated. This effect passes throughout the body and can result in a heart that is also overstimulated, resulting in an increased heart rate. It can also result in feelings or symptoms of manic, anxiety, and an inability to be still and rest.
The thyroid has a lot to do with the quality of the mind, and an overactive thyroid often contributes to an inability to concentrate or to slow thoughts down. Thyroid disorders can often be misdiagnosed as mental or brain disorders because of how profoundly it impacts mood and stability.
An overactive thyroid can have its roots in hormone overproduction that is due to non-autoimmune reasons (like medication side effects, viral infections, or toxicity), or which are rooted in an immune system gone rogue, when the immune system produces antibodies to attack the thyroid. [tweet_quote]Hormone overproduction from medications can cause an overactive thyroid.[/tweet_quote]
Autoimmune hyperthyroidism is referred to as Graves’ disease. When the immune system is triggered, it attacks the thyroid and causes inflammation that enlarges the gland, resulting in higher levels of thyroid hormones than the body requires.
One of the common symptoms associated with Graves’ disease is an inflamed eye condition referred to as proptosis, where the tissue surrounding the eyes swells and causes the eyeballs to appear to bulge forward. This is reversible if treated early.
Hyperthyroidism and Graves’ disease are diagnosed by blood tests, and are typically treated with radioactive iodine or antithyroid medications.
Hypothyroidism and Hashimoto’s Thyroiditis
Hypothyroidism occurs when the thyroid produces too few hormones, resulting in cells that are not receiving enough energy and end up in a slowed or sluggish state that can include mental symptoms like depression and weight gain without lifestyle changes.
An underactive thyroid can be caused by non-autoimmune reasons such as pregnancy or postpartum hormone changes, viral infections, medication side effects, or other reactions, or can be a result of an immune attack, resulting in autoimmune disease.
Hashimoto’s thyroiditis, or autoimmune hypothyroidism, is the most common autoimmune disorder that exists, impacting roughly 14 million people, although many experts suspect that there are millions of people who are not getting proper diagnoses. (2)
The immune system responds to proteins in the thyroid gland that it mistakenly targets as foreign, slowly destroying the gland. In some people, the thyroid will completely cease to function, but in others, if diagnosed soon enough, autoimmune causes can be treated, and the disease can be paused or sent into remission. The result may be a partially functioning gland.
Hashimoto’s is diagnosed by blood tests, and in some cases, ultrasound or CT scan. It is often treated with lifestyle modifications to remove offending triggers, and can be modulated with thyroid hormone replacement.
Symptoms of Thyroid Dysfunction

The symptoms of a dysfunctional thyroid are wide and varied, and for most, take many years to become fully apparent. It can sometimes take many years, or even a decade, to get a full diagnosis, since symptoms of thyroid disease can overlap with numerous other conditions like rheumatoid arthritis, depression, bipolar disorder, anxiety, and adrenal problems.
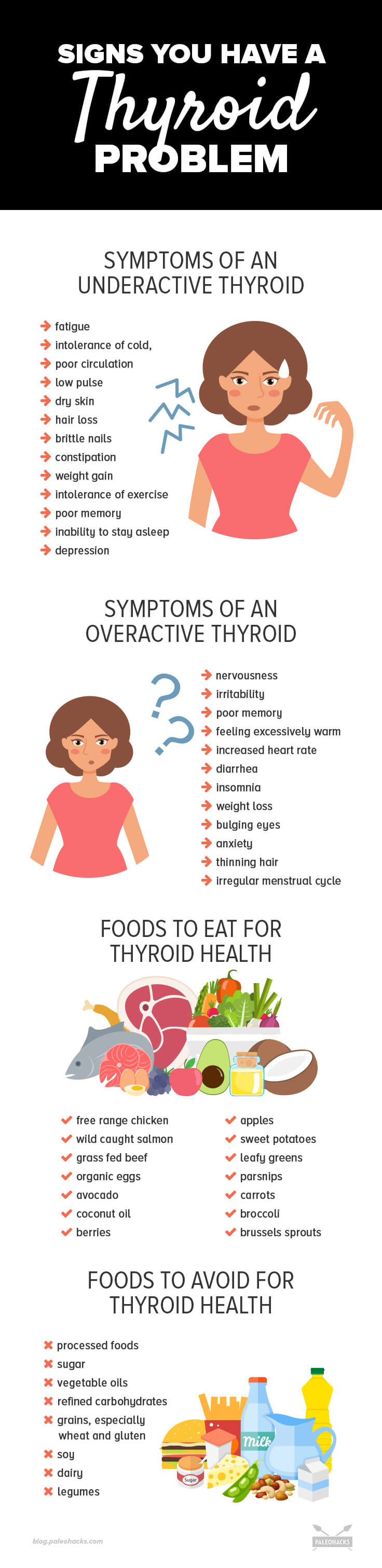
Common symptoms of an underactive thyroid may include:
- Fatigue or excessive tiredness
- Intolerance of cold, or feeling significantly colder than everyone else in the room
- Cold extremities or poor circulation
- Low pulse
- Dry skin
- Hair loss on the head and eyebrows
- Brittle nails
- Constipation
- Weight gain and inability to lose weight
- Intolerance of exercise or exertion
- Poor concentration and memory
- Inability to stay asleep or fall into restful sleep, despite fatigue
- Depression
Symptoms of an overactive thyroid can include:
- Nervousness
- Irritability
- Poor concentration and memory
- Feeling excessively warm, warmer than everyone in the room, or having hot flashes
- Increased heart rate
- Diarrhea or irritable bowels
- Insomnia or inability to relax and fall asleep
- Weight loss without effort
- Bulging eyes
- Anxiety or panic attacks
- Thinning hair
- Reduced or irregular menstrual cycle
For some, many of these symptoms will appear, but for others, only one or two prominent symptoms will appear.
Foods to Eat for Thyroid Health

While there can be conflicting opinions as to which foods are specifically good for the thyroid, the general assumption is that fresh, unprocessed foods are beneficial, while processed foods are best avoided.
A diet rich in clean, free-range proteins, healthy fats, and vegetables and fruits is the best way to naturally support hormone function.
Proteins: The thyroid needs the right amount of protein for blood sugar balance and energy, so it’s essential to consume protein regularly. As a nutritionist who specializes in thyroid conditions, I recommend protein with every meal. 10 to 15 grams of protein is a good baseline, but some people need significantly more.
Fats: Thyroid issues can be triggered by inflammation and can also contribute to increased inflammation. Healthy fats are highly anti-inflammatory, and should be consumed regularly. Coconut oil, avocado oil, and oils from fatty, wild-caught fish should be part of a healing diet for any thyroid disorder.
Carbohydrates: While super low-carb diets may be therapeutic for some conditions, thyroid disorders require carbohydrates. The thyroid requires a certain level of carbohydrates and glucose to synthesize hormones. While these can primarily be achieved from vegetables and fruits, they should be consumed in higher quantities than are typically found in low-carb or ketogenic diets.
Foods to Avoid for Thyroid Health
Goitrogens get a bad rap in the thyroid community because they are reputed to reduce the thyroid’s ability to make hormones. The thyroid needs iodine, and it is suggested by some thyroid practitioners that goitrogens interfere with the ability of the thyroid to access iodine.
Foods that are considered to be goitrogens include cruciferous vegetables like broccoli, cabbage, cauliflower, and Brussels sprouts. Other goitrogens are flax seeds, peanuts, soy, spinach, strawberries, and sweet potatoes.
Dr. Datis Kharrazian, a well-respected expert in the thyroid community, explains that thyroid enlargement is not caused by goitrogens in foods, but rather from inflammation in general. Unfortunately, many thyroid patients avoid eating all goitrogens and miss out on the anti-inflammatory benefits of cruciferous vegetables, which also help to remove toxins and chemicals from the body that can, in some cases, be causes of autoimmunity in the first place.
Instead of avoiding these healthy vegetables, thyroid patients should instead focus on avoiding foods that can trigger immune sensitivity and cause inflammation. These foods can include:
- Processed foods of any kind
- Sugar (even natural and artificial sweeteners)
- Vegetable oils
- Refined carbohydrates
- Grains, especially wheat and gluten
- Soy
- Dairy
- Legumes
Because the Paleo diet naturally excludes many of these foods already, it has become a go-to therapeutic food plan for anyone suffering from thyroid conditions.
Lifestyle Factors and Thyroid Health
The thyroid – and all endocrine organs – are extremely sensitive to sources of toxins and chemicals. While food can be a major source of this, chemicals from cosmetics, environmental sources, households, work spaces, and numerous other outside sources can accumulate in the body and contribute to inflammation, chronic conditions, and hormone imbalances.
When it comes to addressing thyroid health, it’s best to avoid synthetic ingredients of all kinds – especially in cosmetics or personal care products that touch the skin and can get absorbed.
Supplements for Thyroid Health

While some supplements can definitely be beneficial, it’s essential to run any supplements by a practitioner who is skilled in thyroid wellness. Below I’ve addressed some of the most common supplements recommended for thyroid conditions.
Iodine: Many holistic practitioners recommend iodine to anyone with symptoms of thyroid disorders. This practice should be seriously questioned, however, since supplemental iodine can worsen autoimmunity. When iodine is consumed naturally from food sources, like sea vegetables, it can be highly beneficial. But in supplement form, when it lacks the other whole food components, it can increase inflammation in the thyroid.
Selenium: Selenium is one of the nutrients required by the thyroid to synthesize hormones. It is found naturally in foods like Brazil nuts, sardines, grass-fed beef, and chicken. It could be argued that anyone eating a Paleo diet will consume an ample amount of food-sourced selenium and does not need to take extra. However, in some cases of extreme deficiency, a practitioner may recommend a short course of supplemental selenium.
Magnesium: A mineral that is a common deficiency, magnesium is required for the conversion of T4 into the active T3. Without enough magnesium, thyroid hormone levels will likely not appear normal. Magnesium is found in foods such as leafy greens, avocado, dark chocolate, and seafood, and again, will typically be regularly consumed on a Paleo diet. But since deficiency is common, a high-quality magnesium citrate or magnesium glycinate supplement can often be beneficial for thyroid conditions.
Turmeric: Highly anti-inflammatory, turmeric is a potent medicinal supplement and food that is often beneficial for chronic conditions, including thyroid disorders. While it’s not safe for everyone (pregnant women and those on blood thinners should not take turmeric), it can be integrated into the diet and does not necessarily need to be consumed in capsule form.
Medication & Hormone Replacement
Many thyroid conditions are treated medically. For some, this can take the edge off of numerous unpleasant and life-altering symptoms, but when thyroid problems are due to autoimmunity, medication alone will not be enough to reverse or completely remove symptoms.
Graves’ disease or hyperthyroidism can often be treated with thyroid blockers or radioactive iodine to downregulate the thyroid’s hormone production. [tweet_quote]Hormone replacement therapy can help treat hyperthyroidism.[/tweet_quote]
Hypothyroidism or Hashimoto’s thyroiditis can often be treated with thyroid hormone replacement. There are a number of prescription medications available, most of which are either T3 or T4 (or a combination of both). Thyroid medication dosing is a temperamental process and there is rarely a one-size-fits-all dosage that works. Thyroid patients need regular monitoring of their levels to ensure that dosage is meeting needs, and not artificially creating hyperthyroid conditions.
Hormone replacement is often a long-term process, especially when Hashimoto’s has destroyed part or all of the thyroid. It’s essential for thyroid patients to work with their practitioner to find a hormone replacement plan that makes them feel well. Sometimes one medication won’t work, and the patient will actually feel worse. Expert thyroid practitioners will use their patients’ feelings as well as lab results to seek out a hormone replacement plan that is effective.
7-Day Thyroid Meal Plan
Day 1
Breakfast: Zucchini Fritters with Kale and Mushroom Sausage Patties
Lunch: Sweet Honey-Baked Salmon with Baked Butternut Squash
Dinner: Crockpot Rosemary Citrus Chicken with Cauliflower Mashers
Day 2
Breakfast: Salmon Eggs Benedict with Sweet Potato Muffins
Lunch: Rainbow Turkey Salad
Dinner: Coconut-Crusted Chicken Fingers with No Potato Salad
Day 3
Breakfast: Savory Zucchini Pancakes with Bacon and Chives
Lunch: Chicken Mango Lettuce Wraps
Dinner: Avocado Bacon Burger with Cajun Sweet Potato Fries
Day 4
Breakfast: Double-Meat Breakfast Burrito
Lunch: Salmon Burgers with Mango Jicama Slaw
Dinner: Crockpot Chicken and Cauliflower Rice Soup with Paleo Dinner Rolls
Day 5
Breakfast: Prosciutto-Wrapped Asparagus Dipped in Soft-Boiled Eggs
Lunch: Taco Soup with Ground Beef
Dinner: One-Pan Maple Dijon Chicken and Brussels Sprouts
Day 6
Breakfast: Bacon and Spinach Frittata
Lunch: One-Pan Lemon and Herb Chicken
Dinner: Mashed Garlic Cauliflower and Meatballs with Roasted Asparagus
Day 7
Breakfast: BLT Breakfast
Lunch: Mushroom-Onion Hasselback Chicken with Brussels Sprout and Apple Salad
Dinner: Tangy Sweet Pork Chops with Beet Purée
(Read This Next: The Thyroid-Sleep Connection)



 10 Minute HIIT Wall Workout
10 Minute HIIT Wall Workout





Show Comments